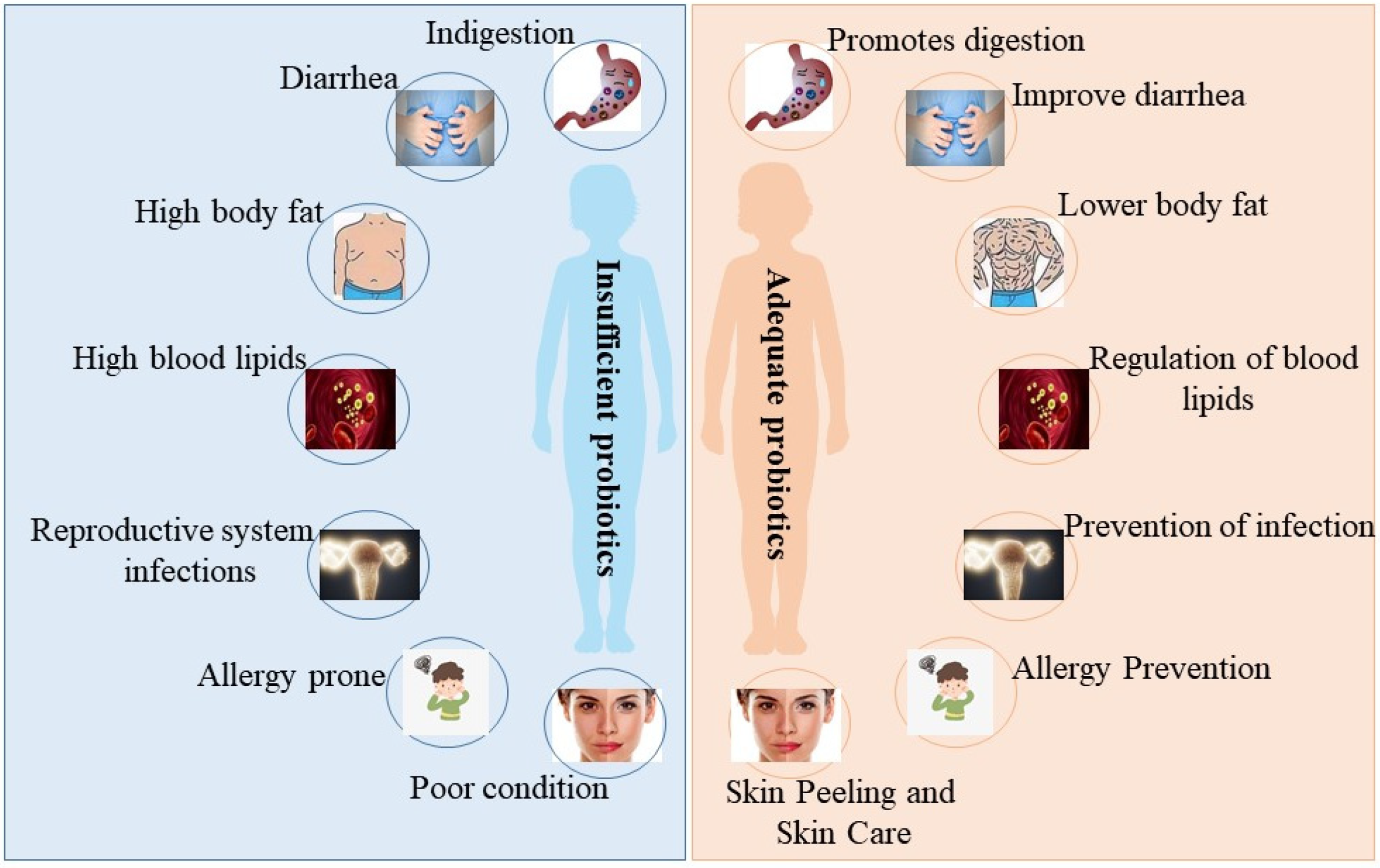
Understanding the Gut Microbiome and Antibiotic Impact
The human gut hosts a complex and dynamic ecosystem of trillions of microorganisms collectively known as the gut microbiome. This community plays a pivotal role in digestion, immune function, mental health, and overall well-being. However, when antibiotics are administered to fight bacterial infections, they often do not discriminate between harmful pathogens and beneficial bacteria. This can result in significant disruption of the microbiome, leading to various gastrointestinal issues, including diarrhea, bloating, and dysbiosis—a state where harmful microbes outnumber beneficial ones.
Given this disruption, many turn to probiotics as a strategy to restore their gut health. But the role of probiotics in post-antibiotic recovery is nuanced and has garnered both support and skepticism in scientific and medical circles. Understanding whether probiotics are beneficial or potentially harmful requires delving into recent research and clinical insights.
The Potential Benefits of Probiotics in Gut Recovery
Probiotics are live microorganisms that, when consumed in adequate amounts, confer health benefits to the host. They are commonly found in fermented foods like yogurt, kefir, sauerkraut, and in supplement form. Several studies suggest that probiotics can aid in re-establishing a healthy microbial balance after antibiotic treatment.
- Restoration of Microbial Diversity: Certain probiotic strains can help repopulate the gut with beneficial bacteria, thus enhancing microbial diversity, which is a marker of a healthy microbiome.
- Reduction of Antibiotic-Associated Diarrhea: Multiple clinical trials have shown that probiotics can significantly reduce the incidence and severity of diarrhea linked to antibiotic use.
- Supporting Immune Function: Probiotics may bolster the immune response, which can be suppressed during and after antibiotic treatment.
- Alleviation of Gastrointestinal Symptoms: Many users report relief from bloating, gas, and discomfort when incorporating probiotics post-antibiotic therapy.
All these benefits highlight a promising avenue for mitigating some of the negative effects of antibiotics on gut health. However, it’s important to recognize that probiotics are not a one-size-fits-all solution, and their effectiveness can vary based on individual health status, microbiome composition, and the strains used.
Challenges and Risks: When Probiotics Might Hinder Gut Recovery
While probiotics offer potential benefits, recent research, such as the findings discussed in ), indicate that probiotics can sometimes hinder gut recovery or even make symptoms worse for certain individuals.
- Strain Specific Effects: Not all probiotic strains are beneficial for everyone. Some strains may not colonize or persist in the gut, rendering them ineffective or even leading to negative interactions.
- Potential for Overgrowth: In immunocompromised individuals or those with compromised gut barriers, probiotics can sometimes lead to bacterial overgrowth or infection.
- Disruption of Native Microbiota: Introducing new strains might interfere with the existing microbiome, preventing the natural recovery process or causing imbalance.
- No Universal Solution: The ‘one-size-fits-all’ approach is flawed. What works for one person may be ineffective or harmful to another.
Furthermore, some scientific studies and experts argue that indiscriminate use of probiotics without personalized assessment can be counterproductive, emphasizing the need for tailored approaches and caution when incorporating probiotics post-antibiotics.
The Science Behind Personalized Probiotic Therapy
Why One Probiotic Does Not Fit All
The gut microbiome is highly individualized, influenced by genetics, diet, environment, age, health status, and prior microbial exposure. Recent insights suggest that probiotic supplementation should be carefully selected based on these factors rather than adopting generic probiotic products.
For example, a person with a healthy baseline microbiome might not benefit from probiotic supplements and may even experience disruptions, while someone with severe dysbiosis might require targeted microbial therapy. Advanced diagnostics, such as microbiome sequencing, are increasingly used to identify specific deficiencies and guide personalized probiotic regimens.
The Growing Evidence and Future Directions
Current research emphasizes that prebiotics, which are dietary fibers that stimulate the growth of beneficial bacteria, alongside specific probiotics, may offer a more effective approach for gut recovery. Additionally, postbiotics—metabolic byproducts of probiotics—are gaining attention for their potential benefits without the risks associated with live bacteria.
Scientists advocate moving away from broad, commercial probiotic products toward tailored microbiome therapeutic strategies designed for individual needs.
Practical Recommendations for Gut Recovery Post-Antibiotics
If you’re recovering from antibiotics and considering probiotic use, keep these points in mind:
- Consult Healthcare Professionals: Before starting any probiotic supplement, discuss with a healthcare provider, especially if you have underlying health conditions or are immunocompromised.
- Choose Strain-Specific Supplements: Opt for products with well-researched strains supported by clinical evidence for post-antibiotic recovery.
- Prioritize Diet: Incorporate fermented foods and dietary fibers to naturally support beneficial bacteria.
- Monitor Your Response: Keep track of symptoms and microbiome health markers to assess effectiveness and adjust as needed.
- Avoid Overuse of Probiotics: Using probiotics excessively or without guidance can be detrimental; moderation and professional advice are key.
Remember, restoring gut health is a gradual process that involves diet, lifestyle, and personalized interventions, not solely relying on supplements.
Conclusion
In summary, probiotics can be a valuable tool in promoting gut recovery after antibiotic treatment, but their use must be approached with caution and personalized understanding. While some strains may support microbial diversity and reduce symptoms, others may not be suitable for every individual and could even impede recovery. Ongoing research continues to unravel the complexities of the gut microbiome and the optimal ways to restore it. The future of post-antibiotic gut health management likely lies in precise, individualized probiotic therapies based on detailed microbiome analysis.
Always remember: The key to successful gut recovery is a balanced, personalized approach that combines diet, lifestyle, and, when necessary, targeted microbial interventions under professional guidance.
For more updated news please keep visiting Hourly Prime News.