The Growing Concern of Obesity and Its Mental Health Implications
Obesity has long been recognized as a significant health concern due to its association with cardiovascular diseases, diabetes, and metabolic syndromes. However, recent research sheds light on a lesser-known but equally alarming consequence: its profound impact on mental health, especially anxiety and cognitive decline. As obesity rates continue to climb globally, understanding its far-reaching effects on brain health becomes essential for developing comprehensive prevention and treatment strategies.
How Obesity Contributes to Anxiety Disorders
The Biological Link Between Obesity and Anxiety
Multiple studies suggest that obesity can contribute to the development of anxiety disorders. The underlying mechanisms involve complex biological pathways, including hormonal imbalances, inflammatory responses, and alterations in brain chemistry.
- Inflammation: Excess adipose tissue in obese individuals leads to increased levels of pro-inflammatory cytokines. Chronic inflammation has been associated with alterations in neurotransmitter function, notably serotonin and dopamine, which play crucial roles in regulating mood and anxiety.
- Hormonal Changes: Obesity disrupts hormonal balance, particularly increasing cortisol levels due to heightened stress response. Elevated cortisol levels are known to exacerbate anxiety symptoms.
- Neurochemical Alterations: Obesity may alter the functioning of neurotransmitters such as gamma-aminobutyric acid (GABA) and glutamate, which are vital in maintaining neuronal stability and preventing excessive anxiety responses.
Psychological and Social Factors
Beyond biological mechanisms, social stigma and psychological distress related to obesity can significantly elevate anxiety levels. Individuals facing societal discrimination often experience lowered self-esteem, social withdrawal, and heightened stress responses, all contributing to anxiety disorders.
Cognitive Impairment and Obesity: An Emerging Concern
The Cognitive Decline in Obese Individuals
There’s growing evidence indicating that obesity is not only linked to physical health problems but also to cognitive impairment. This impairment can range from mild forgetfulness to severe deficits impacting daily functioning.
- Memory and Learning: Obesity has been associated with reduced hippocampal volume, the brain region critical for learning and memory formation.
- Executive Function: Tasks involving decision-making, problem-solving, and impulse control often become more challenging for obese individuals, possibly due to disrupted prefrontal cortex activity.
- Processing Speed: Cognitive processing speed tends to decline with increased adiposity, affecting overall mental agility.
Mechanisms Behind Cognitive Decline
The pathways linking obesity and cognitive decline are multifactorial:
- Vascular Factors: Obesity contributes to atherosclerosis and hypertension, impairing cerebral blood flow.
- Inflammatory Processes: As with anxiety, chronic inflammation damages neural tissue, reducing cognitive function.
- Insulin Resistance: Obese individuals often develop insulin resistance, which has been linked to decreased neuroplasticity and neurodegeneration.
The Role of Lifestyle and Interventions
Importance of Weight Management
Addressing obesity through lifestyle modifications such as diet, exercise, and behavioral therapy can significantly reduce the risk of developing anxiety and cognitive deterioration. Weight loss has been shown to decrease systemic inflammation, improve hormonal balance, and restore brain function.
Psychological Support and Medical Treatments
Integrated approaches that combine mental health support with physical health interventions are crucial. Cognitive-behavioral therapy (CBT) can help manage anxiety symptoms, while pharmacotherapy might be necessary in severe cases. Encouraging physical activity not only aids weight loss but also improves mental health by releasing endorphins and enhancing neurotransmitter levels.
Preventive Strategies and Future Perspectives
Preventing obesity-related mental health issues requires a multifaceted approach:
- Public Awareness: Educating the public about the mental health toll of obesity can motivate healthier lifestyle choices.
- Early Detection: Screening for anxiety and cognitive decline in obese patients allows for timely interventions.
- Research Advancement: Further studies are needed to unravel the precise biological pathways and identify new therapeutic targets.
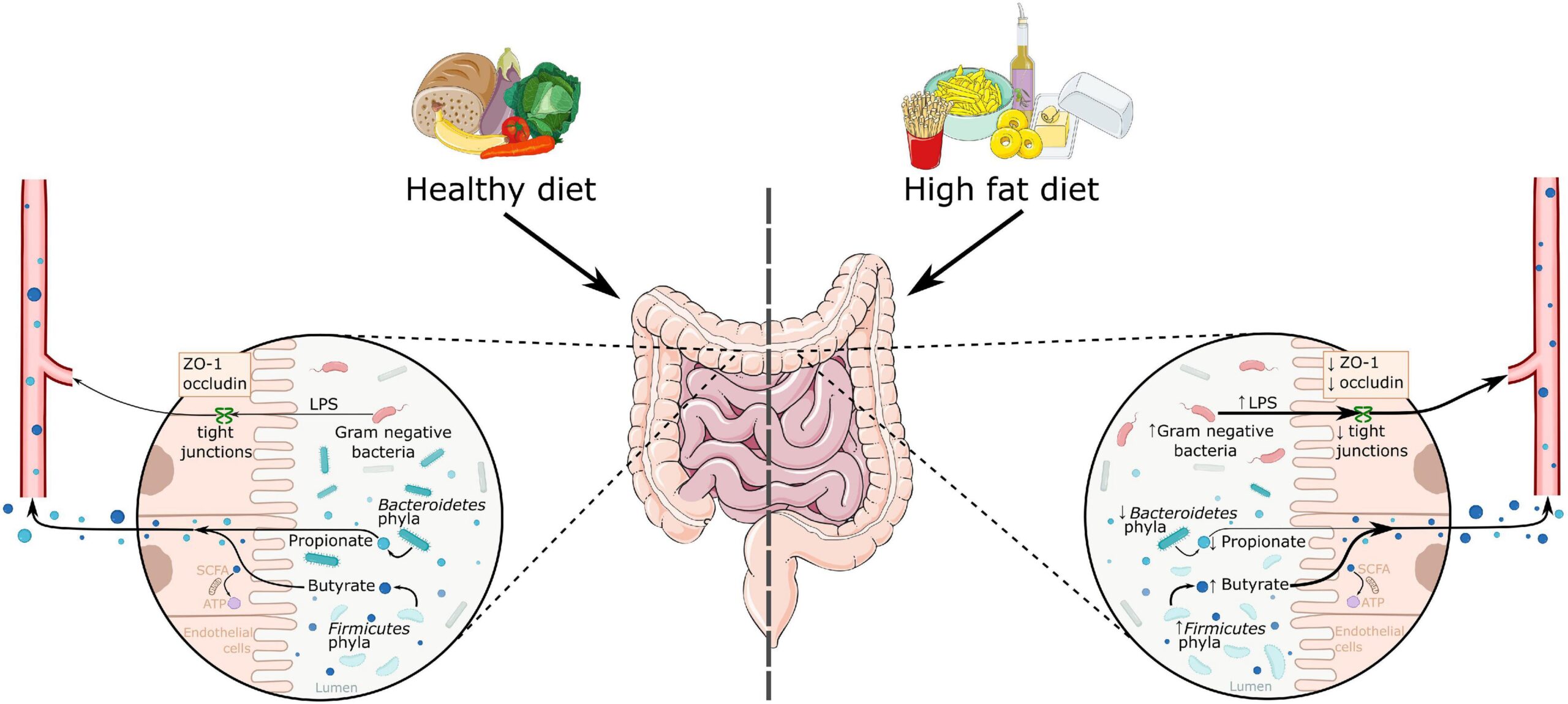
Moreover, emerging research exploring the gut-brain axis indicates that gut microbiota alterations in obese individuals may influence mood and cognition, opening new avenues for treatment through probiotics, diet modifications, and personalized medicine.
Conclusion
The escalating epidemic of obesity poses significant risks not just to physical health but also to mental well-being. The strong association between obesity, anxiety, and cognitive decline emphasizes the importance of adopting holistic health strategies. Combating obesity involves more than just physical health management; it requires addressing the psychosocial and neurobiological consequences that accompany excess weight. By integrating lifestyle changes, medical treatment, and psychological support, we can better safeguard individuals’ mental health and improve their overall quality of life.
Remember: Tackling obesity today can prevent a cascade of mental health challenges tomorrow. Proactive measures and continued research are vital in mitigating these impacts and promoting healthier, more resilient communities.
For more updated news please keep visiting Hourly Prime News.