The Overlooked Connection Between PCOS and Obesity
Obesity has become a global health epidemic, impacting millions across all age groups and backgrounds. While lifestyle factors such as diet and physical activity are commonly blamed, emerging research suggests that underlying medical conditions often go unnoticed—especially Polycystic Ovary Syndrome (PCOS). Though traditionally associated with reproductive health issues, PCOS is increasingly recognized as a significant contributor to obesity and metabolic disturbances. Despite its prevalence, many individuals and even healthcare providers struggle to accurately diagnose PCOS, which delays effective treatment strategies and exacerbates the challenge of weight management.
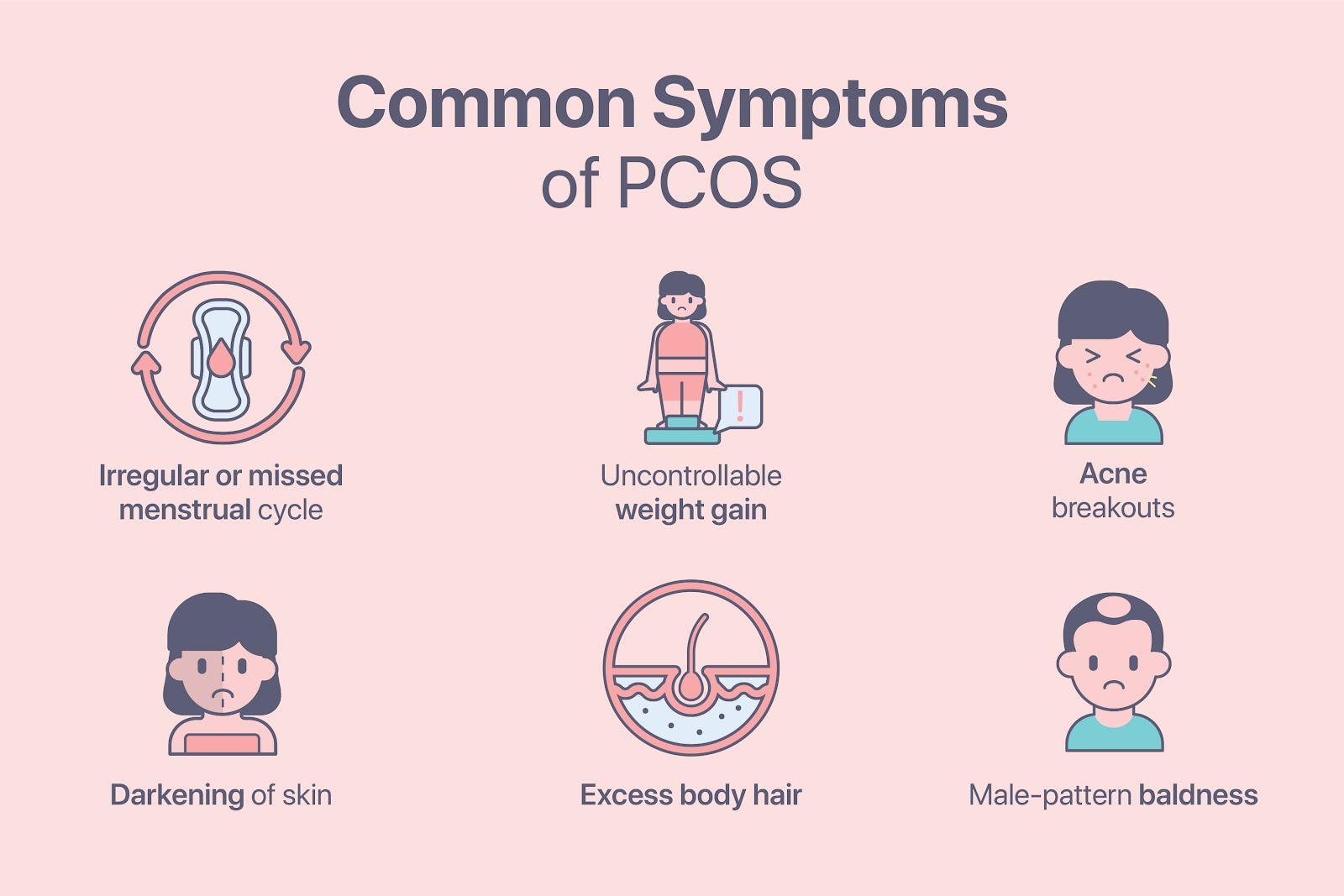
Understanding PCOS: More Than Just a Reproductive Disorder
Polycystic Ovary Syndrome (PCOS) is a complex hormonal disorder affecting women of reproductive age. According to sources such as Medscape, it involves an imbalance of reproductive hormones, specifically elevated androgens, insulin resistance, and the presence of ovarian cysts. The condition’s symptoms can vary widely, often making diagnosis tricky and elusive.
The Silent Link Between PCOS and Obesity
Insulin Resistance as the Heart of the Issue
One of the key factors linking PCOS to obesity is insulin resistance. In women with PCOS, the body’s cells become less responsive to insulin, prompting the pancreas to produce more insulin. Elevated insulin levels not only exacerbate hormonal imbalances but also stimulate excess fat storage, particularly around the abdomen. This creates a vicious cycle: obesity worsens insulin resistance, and insulin resistance further promotes weight gain. Several studies, including those highlighted by Cedars-Sinai, emphasize that women with PCOS often struggle with unexplained weight gain despite diet and exercise efforts.
Hormonal Imbalance and Metabolic Disarray
High levels of androgens (male hormones) present in women with PCOS can contribute to increased fat deposition and difficulty losing weight. Moreover, hormonal imbalances influence appetite regulation, favoring increased hunger and cravings. The hormonal chaos extends beyond reproductive effects to affect overall metabolism, predisposing affected women to cardiovascular disease, type 2 diabetes, and severe obesity. The recognition that PCOS is not merely reproductive but also a metabolic disorder underscores the importance of comprehensive diagnosis and management.
Challenges in Diagnosis: Why Is PCOS Often Missed?
Despite its prevalence, PCOS remains a frequently misdiagnosed or underdiagnosed condition. Multiple sources, such as Medscape and The Australian, many women find their symptoms dismissed or misunderstood.
The diagnostic process can be complicated because features such as irregular periods, cyst presence, and androgen excess vary widely. An international study from CU Anschutz confirms that many patients with PCOS report feeling dismissed, misunderstood, and frustrated about their health, further delaying diagnosis.
The Importance of Awareness and Comprehensive Testing
Early recognition of PCOS can significantly improve health outcomes. Given that symptoms often overlap with other conditions, healthcare providers must consider PCOS as a primary diagnosis when women present with unexplained weight gain, hormonal imbalances, or metabolic disturbances.
- Blood tests assessing androgen levels, insulin resistance markers, and ovarian function.
- Ultrasound scans to detect ovarian cysts and morphological features.
- Assessment of lifestyle factors, including diet, physical activity, and stress levels.
- Holistic management approaches, combining hormonal therapy, lifestyle modifications, and metabolic health treatments.
Implications for Women Struggling With Obesity and PCOS
Women with PCOS often find themselves trapped in a cycle of weight gain and failed weight-loss attempts. Understanding the condition’s underlying causes shifts the focus from merely dieting to addressing hormonal and metabolic health. Approaches such as insulin-sensitizing medications (like Metformin), targeted dietary plans, and regular physical activity tailored to their needs can help mitigate some of these issues.
Psychological and Social Factors
Many women report feelings of frustration, stigma, and emotional distress related to their weight and reproductive health challenges. The stigma surrounding obesity can compound feelings of shame and guilt, delaying seeking medical help. It’s essential to promote awareness that PCOS is a complex, multifaceted disorder requiring compassionate, individualized treatment plans.
Final Thoughts: Bridging the Gap in Awareness and Treatment
As emerging research continues to shed light on the hidden links between PCOS and obesity, the urgency to improve diagnosis rates and treatment options becomes clearer. Both women and healthcare providers must be informed about the nuanced symptoms and the importance of early intervention. Recognizing PCOS as a metabolic disorder with reproductive consequences can transform outcomes for countless women battling weight challenges.
Increased awareness, comprehensive testing, and personalized management can empower women to take control of their health and break free from the cycle of obesity linked to PCOS.
Conclusion
Understanding the silent yet significant role of PCOS in obesity is key to addressing the global health challenge effectively. By shifting the perspective from lifestyle-only views to incorporating hormonal and metabolic health, we can pave the way for better diagnosis, treatment, and ultimately, improved quality of life for women affected worldwide.
For more updated news please keep visiting Hourly Prime News.