Adolescence is a critical period characterized by significant physiological, psychological, and social changes. During this stage, individuals become more susceptible to various infectious diseases, including *Invasive Meningococcal Disease (IMD)*, a severe bacterial illness that can lead to meningitis, sepsis, and potentially fatal outcomes. The importance of *timely prevention* cannot be overstated, as early intervention significantly reduces the risk of outbreaks and long-term health consequences. In this comprehensive overview, we will explore the nature of adolescent IMD, its risk factors, current prevention strategies, and how healthcare providers, educators, and parents can collaborate to protect adolescents effectively.
Understanding Invasive Meningococcal Disease in Adolescents
What is Invasive Meningococcal Disease?
Invasive Meningococcal Disease is caused by the bacterium *Neisseria meningitidis.*, which colonizes the nasopharynx of healthy carriers. While many individuals harbor the bacteria asymptomatically, certain conditions can lead to its invasive progression, resulting in life-threatening conditions such as meningitis (infection of the membranes surrounding the brain and spinal cord) and septicemia (bloodstream infection). The disease progresses rapidly and requires prompt medical attention.
Why are Adolescents Particularly at Risk?
Adolescents are especially vulnerable to IMD due to several عوامل, including:
- High carriage rates: Adolescents have increased social interactions in settings like schools, colleges, and social gatherings, facilitating bacterial transmission.
- Immune system maturity: The adolescent immune response can sometimes be inadequate to fend off the bacteria, especially if previously unvaccinated.
- Behavioral factors: Certain behavioral habits such as smoking or close-contact sports may increase susceptibility.
Significance of Timely Prevention
The Impact of Delay in Prevention
Delaying vaccination or overlooking early preventive measures can lead to outbreaks that are difficult to control and may result in severe health outcomes. Timeliness in prevention is linked to:
- Reduced incidence: Prevents the occurrence of disease altogether.
- Decreased mortality and morbidity: Lessens the risk of death and long-term neurological damage.
- Lower healthcare costs: Avoids costly hospitalizations and complex treatments.
Current Recommendations for Prevention
Health authorities like the European Medical Journal emphasize a multifaceted approach that includes vaccination, awareness, and early detection strategies.
Prevention Strategies for Adolescent IMD
1. Vaccination: The Cornerstone of Prevention
Vaccination remains the most effective method to prevent invasive meningococcal disease. Several vaccines target different *Neisseria meningitidis* serogroups (A, B, C, W, Y), with recommendations tailored to age groups and regional epidemiology.
- Quadrivalent conjugate vaccines: Cover serogroups A, C, W, and Y. Widely recommended for adolescents to provide broad protection.
- Serogroup B vaccines: Specifically designed to prevent serogroup B infections, which are prevalent in certain regions.
- Vaccination schedules: Typically administered in a series of doses during adolescence, ideally before college entry or social mixing.
Healthcare providers should ensure that adolescents are up-to-date with the latest vaccination schedules and are aware of the importance of booster doses to sustain immunity.
2. Raising Awareness and Education
Knowledge dissemination plays a vital role in prevention. Educating adolescents, parents, and educators about:
- The signs and symptoms of IMD
- The importance of vaccination
- Hygiene practices to reduce transmission
Encouraging open conversations about vaccination hesitancy and debunking myths can improve vaccine uptake rates and foster a proactive attitude toward prevention.
3. Early Detection and Rapid Response
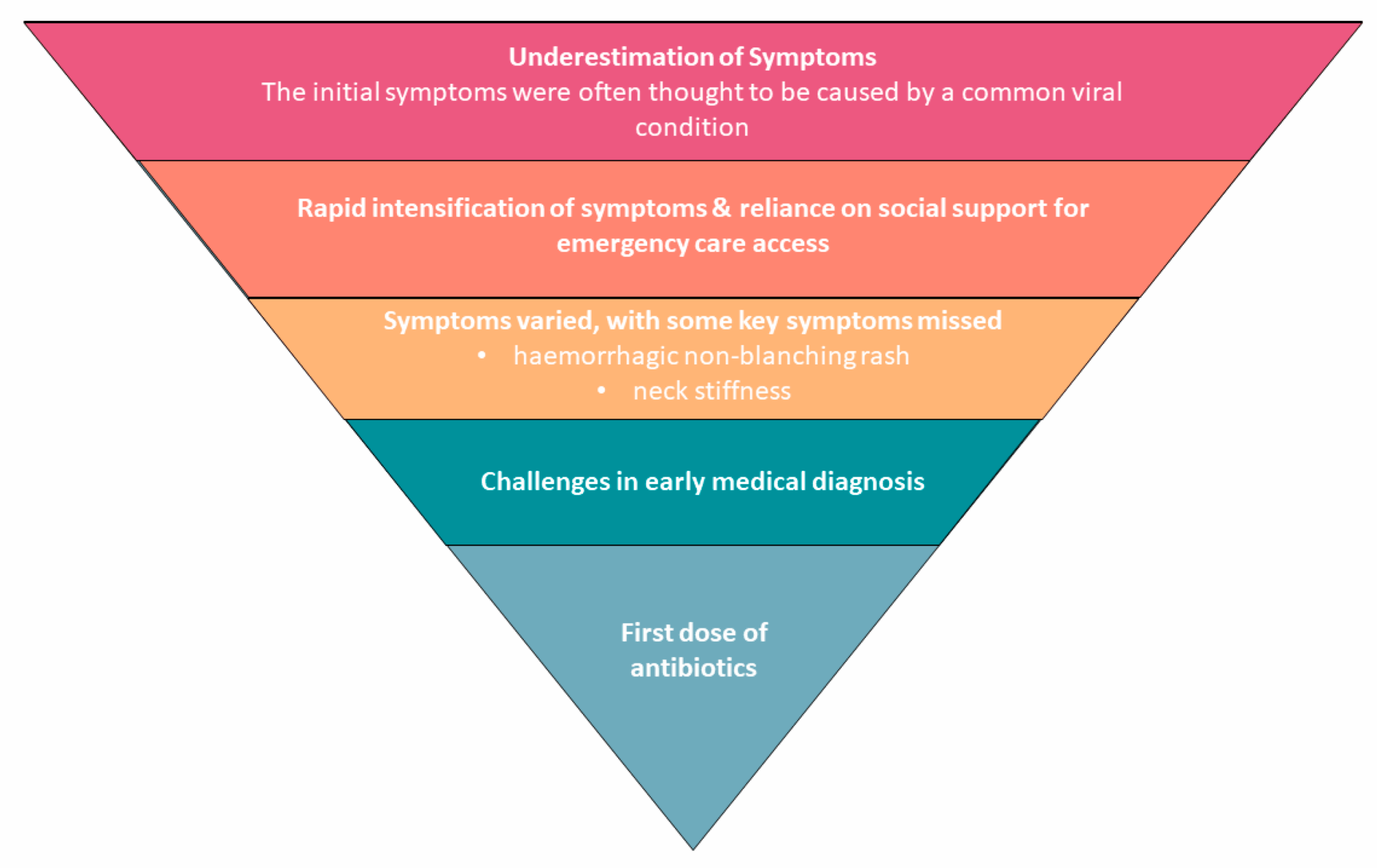
Timeliness in recognizing symptoms such as sudden fever, headache, neck stiffness, rash, and confusion can be lifesaving. Schools and healthcare providers should maintain vigilance and ensure prompt referral for medical evaluation when symptoms arise.
4. Addressing Behavioral and Environmental Factors
Reducing risk behaviors like smoking and promoting good hygiene practices can decrease carriage and transmission of the bacteria. Additionally, minimizing overcrowding in schools and communal areas can lower exposure risks.
Implementing a Collaborative Approach
The Role of Healthcare Providers, Schools, and Families
Healthcare providers should actively recommend vaccination during routine visits, especially in adolescence. They must stay updated on emerging vaccine guidelines and regional disease patterns.
Schools and educational institutions can facilitate vaccination campaigns and health education programs. They can also implement policies to identify and manage suspected cases swiftly.
Parents and adolescents should be encouraged to participate in vaccination programs and adopt healthy behaviors. Awareness campaigns tailored towards young populations can empower them to make informed decisions.
Conclusion
Adolescent invasive meningococcal disease poses a significant public health challenge, but with timely and strategic prevention efforts, the risks can be substantially mitigated. Vaccination remains the cornerstone, complemented by education, early detection, and behavioral modifications. A concerted effort involving healthcare providers, schools, families, and policymakers is essential to safeguard adolescent health and prevent outbreaks.
By prioritizing timely prevention strategies now, we can protect future generations from the devastating effects of IMD and build healthier communities.
For more updated news please keep visiting Hourly Prime News.