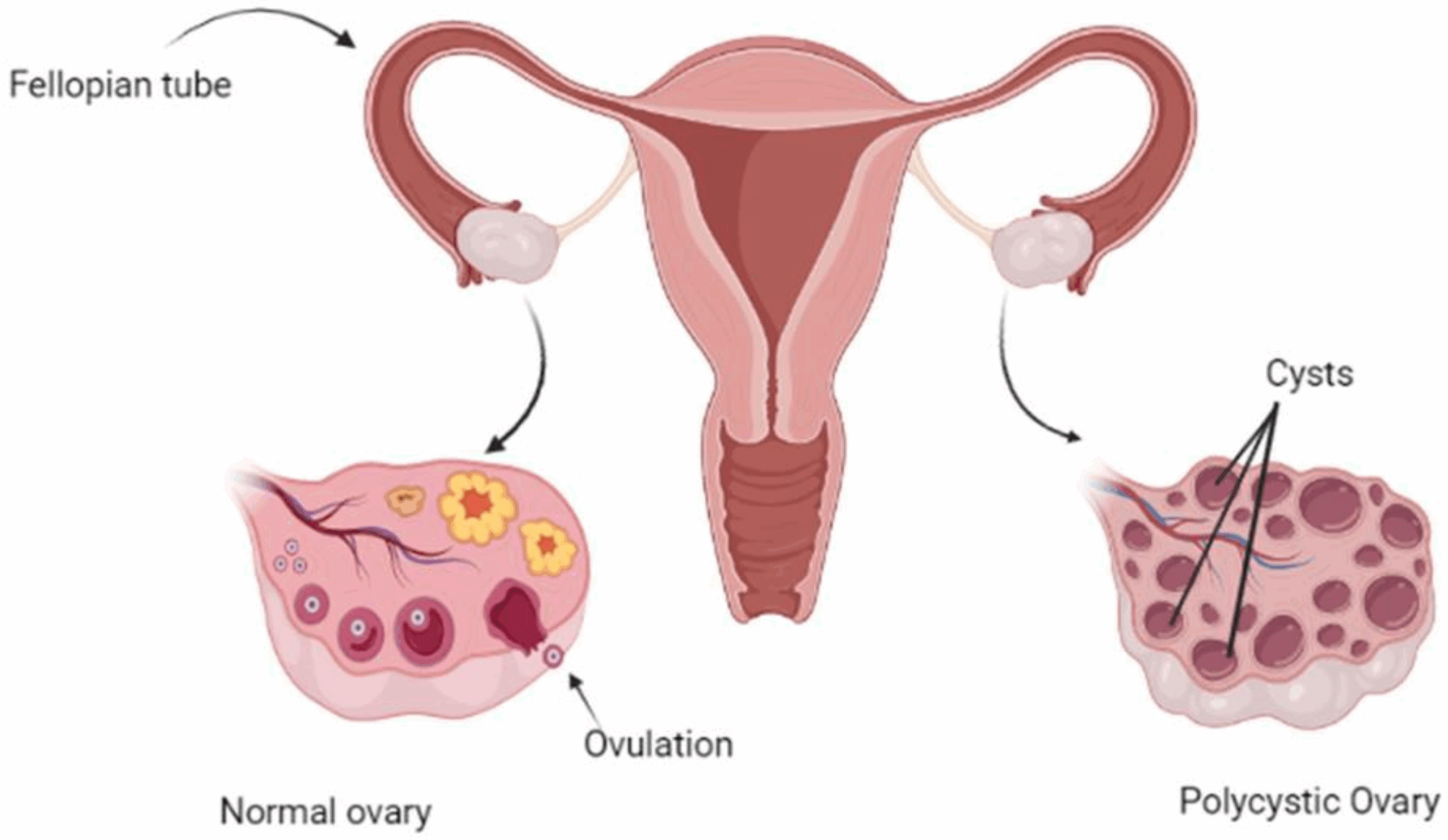
Understanding the Role of Genetics in PCOS
Polycystic Ovary Syndrome (PCOS) is a complex hormonal disorder affecting millions of women worldwide. While lifestyle factors such as diet, stress, and physical activity certainly influence its onset and severity, a growing body of research emphasizes the pivotal role genetics play in shaping its progression. Recent studies highlight that PCOS is not solely a product of environmental influences but also has a significant hereditary component that dictates how the syndrome manifests and evolves over time.
Genetic predisposition can influence various aspects of PCOS, including hormonal imbalances, ovarian function, insulin resistance, and even susceptibility to associated metabolic conditions. Understanding these genetic factors provides vital insights into early diagnosis, personalized treatment, and preventative strategies for women at risk of developing PCOS.
Genetics and the Onset of PCOS
Research indicates that women with a family history of PCOS are more likely to develop the condition themselves, suggesting an inherited component. Specific genes involved in hormonal regulation, ovarian development, and insulin signaling pathways have been identified as potential contributors.
For example, variations in genes such as DENND1A, THADA, and FTO have been linked to increased risk of PCOS. These genes potentially influence androgen production, follicular development, and metabolic regulation—factors central to the syndrome’s onset. Genetic studies reveal that women carrying certain alleles of these genes tend to develop symptoms earlier or with greater severity.
Importantly, the genetic predisposition interacts with environmental factors, meaning that women with such genetic variants are more susceptible when exposed to lifestyle stressors like poor diet or high stress levels. Nonetheless, they provide a biological foundation that predisposes women to PCOS even before clinical symptoms appear.
Genetic Influences on PCOS Progression and Severity
Beyond the onset, genetics also play a crucial role in how PCOS progresses and manifests over time. Some women may experience more severe symptoms, including profound hormonal imbalances, metabolic disturbances, or infertility. These variations are often rooted in genetic differences that affect ovarian response, insulin sensitivity, and androgen excess.
For instance, genetic variants affecting insulin receptor function can lead to insulin resistance, a common feature in PCOS. This resistance exacerbates hyperandrogenism and may accelerate the progression of symptoms such as hirsutism, acne, and metabolic syndrome. Conversely, other genetic profiles might confer a milder disease course, emphasizing the importance of personalized approaches to management based on genetic makeup.
Epigenetics and Environmental Interplay
While genetic makeup provides the blueprint, epigenetic factors—such as DNA methylation and histone modification—modulate gene expression without altering the underlying DNA sequence. Environmental stressors like poor nutrition, stress, and sedentary lifestyles can influence epigenetic marks, thereby impacting PCOS development and progression.
This dynamic interplay suggests that even women with genetic susceptibility can modify disease trajectory through lifestyle changes. For example, interventions targeting insulin sensitivity and hormonal regulation may be more effective if tailored to an individual’s genetic and epigenetic profile.
The Importance of Genetic Research in PCOS Management
Advances in genetic research hold promise for future clinical applications, including:
- Early genetic screening: Identifying at-risk women before the onset of symptoms.
- Personalized therapies: Tailoring treatments based on genetic and epigenetic profiles to improve efficacy and reduce adverse effects.
- Understanding comorbidities: Recognizing genetic links with conditions like diabetes, cardiovascular disease, and mental health disorders—common comorbidities in PCOS.
Ongoing studies continue to uncover new genetic variants associated with PCOS, emphasizing that this disorder is multifactorial and heterogenous. Integrating genetic insights with clinical practices will undoubtedly enhance holistic management strategies.
Conclusion: A Future of Personalized Care
In conclusion, genetics form the backbone of PCOS’s complex etiology—shaping its onset, severity, and progression. Recognizing the hereditary component underscores the importance of genetic counseling, early detection, and personalized treatment. As research advances, a future where interventions are tailored to an individual’s genetic profile becomes increasingly attainable, promising better outcomes and quality of life for women affected by PCOS.
By considering both genetic and lifestyle factors, healthcare providers can develop more effective, targeted strategies to combat this widespread condition. Ultimately, understanding the genetic underpinnings empowers women and clinicians alike in managing PCOS proactively and compassionately.