Rheumatic heart disease, primarily resulting from rheumatic fever, remains a significant health concern, especially in developing countries. Traditionally, the diagnosis hinges on clinical presentation and evidence of prior streptococcal infection, but recent research highlights an intriguing and less explored aspect: the neurological manifestations that can precede or accompany cardiac involvement in early adolescents. Understanding these neurological clues can pave the way for early detection and intervention, potentially reducing morbidity and mortality associated with rheumatic carditis.
Understanding Rheumatic Fever and Carditis in Adolescents
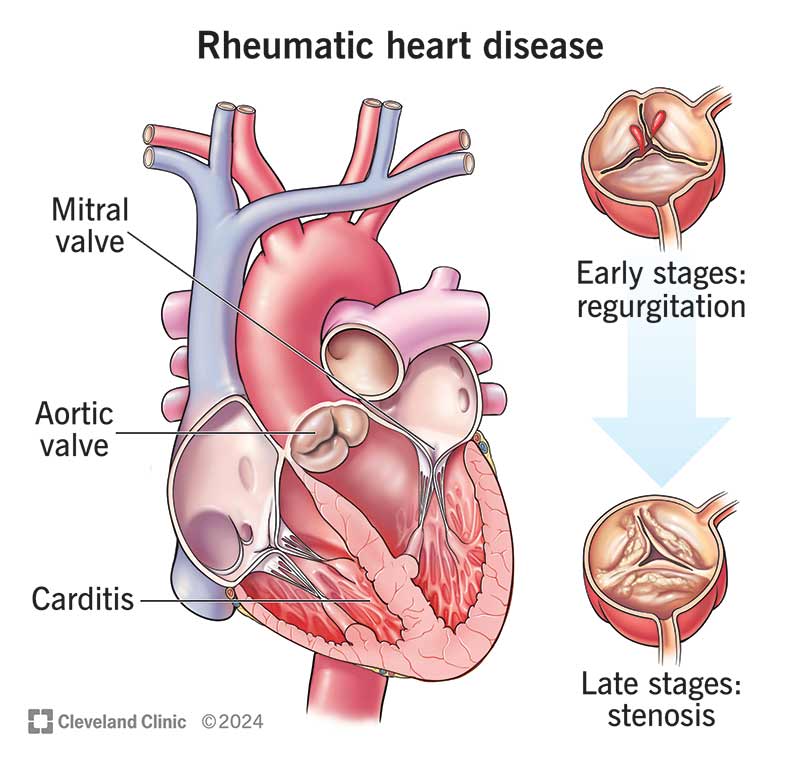
Rheumatic fever is an autoimmune inflammatory disease that occurs as a delayed complication of untreated or inadequately treated group A streptococcal pharyngitis. It can affect multiple organs, including the heart, joints, skin, and brain. Among these, rheumatic carditis is the most severe manifestation, often leading to lifelong cardiac complications such as valvular damage.
In early adolescents, the presentation can sometimes be atypical, with neurological symptoms overshadowing classical signs. This overlap complicates diagnosis, especially when neurological involvement mimics other common conditions like encephalitis or neurological sequelae of infections. Recent case studies underscore the importance of recognizing neurological clues as potential harbingers of rheumatic carditis.
The Link Between Neurological Manifestations and Rheumatic Carditis
One of the intriguing aspects of rheumatic fever is its neurological component, often termed Pandysystic Sydenham’s chorea or simply Sydenham’s chorea—a movement disorder characterized by rapid, involuntary movements, emotional disturbances, and alterations in behavior. Unlike classical cardiac symptoms, neurological signs may appear insidiously, leading clinicians to initially suspect neurological or psychiatric conditions.
Emerging evidence suggests that in some cases, neurological symptoms can be the initial or predominant presentation in early adolescents, even before overt cardiac manifestations become apparent. Recognizing these neurological clues offers a window of opportunity for early diagnosis and management.
Case Studies: Shedding Light on Neurological Clues
A recent publication in Cureus presented two illustrative cases from a tertiary care center in Maharashtra, India, highlighting the significance of neurological clues in diagnosing rheumatic carditis:
- Case 1: An early adolescent boy presented with abrupt onset of involuntary movements, irritability, and emotional lability. No initial cardiac symptoms were evident. Laboratory investigations revealed elevated anti-streptolysin O titers, and echocardiography identified subtle mitral valve regurgitation. This case underscored that neurological signs—particularly chorea—could precede cardiac signs, enabling early diagnosis.
- Case 2: A young girl exhibited neuropsychiatric symptoms alongside mild choreiform movements. Subsequent evaluation demonstrated evidence of rheumatic activity with elevated inflammatory markers and echocardiography confirmed carditis. Notably, her neurological presentation prompted earlier investigation, leading to prompt treatment that mitigated long-term cardiac damage.
These cases exemplify how neurological manifestations serve as vital clues in revealing underlying rheumatic activity in adolescents. Recognizing these signs early can facilitate timely therapy, reducing progression to severe cardiac disease.
Mechanisms Behind Neurological Clues in Rheumatic Fever
The pathophysiology involves an autoimmune process where molecular mimicry causes cross-reactivity between streptococcal antigens and neuronal tissues. This results in inflammation in the basal ganglia, leading to movement disorders such as chorea. Importantly, in adolescents, this neuroimmune response may manifest even before or alongside cardiac inflammation, emphasizing the need for clinicians to maintain vigilance.
Implications for Clinical Practice
Clinicians managing adolescents presenting with neurological symptoms should consider rheumatic fever as a differential diagnosis, especially in high-risk populations. Key considerations include:
- Inquiring about recent streptococcal infections or sore throats.
- Performing appropriate laboratory tests, including anti-streptolysin O (ASO) titers and markers of inflammation.
- Using echocardiography proactively to detect early cardiac involvement even if asymptomatic.
Early diagnosis based on neurological clues can significantly improve outcomes. Initiating anti-inflammatory treatment and antibiotics can halt or slow disease progression, preserving cardiac function.
The Importance of Multidisciplinary Approach
Given the neurological and cardiac overlap, a multidisciplinary approach involving neurologists, cardiologists, and infectious disease specialists is critical. This collaboration ensures comprehensive evaluation and management, optimizing long-term health in adolescents.
Awareness campaigns and clinician education are essential to disseminate knowledge about neurological clues as warning signs. This approach can be especially effective in regions where rheumatic fever remains endemic.
Conclusion
Understanding the neurocardiac connection in rheumatic fever, especially in early adolescents, offers a promising avenue for early detection and intervention. Recognizing neurological clues such as involuntary movements, behavioral changes, and neuropsychiatric symptoms can unmask underlying rheumatic carditis, potentially preventing severe cardiac sequelae. Enhanced vigilance, timely investigations, and a multidisciplinary approach are the cornerstones of improving outcomes in this vulnerable age group.
As highlighted by recent case studies, paying attention to neurological signs not only broadens diagnostic horizons but also emphasizes an integrated approach to adolescent health. The intertwining of neurology and cardiology in rheumatic fever exemplifies the complex yet fascinating nature of autoimmune diseases in the pediatric population.
In sum, early adolescents with neurological manifestations should be evaluated thoroughly for rheumatic activity, especially in endemic areas. This vigilance can be life-changing, ensuring better quality of life and cardiac health preservation.
For more updated news please keep visiting Hourly Prime News.